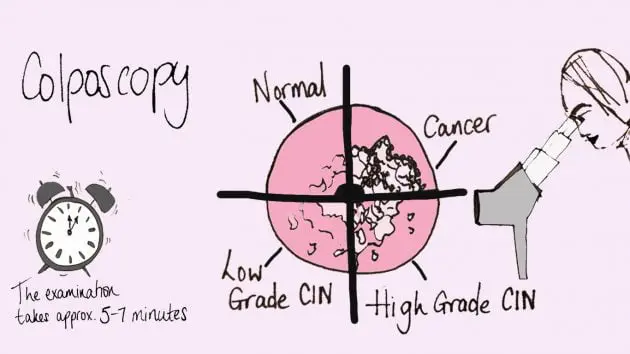
What happens during and after a colposcopy
A colposcopy is a simple outpatient clinic procedure to examine the cervix and it is often performed following an abnormal smear. It allows the specialist to assess the cervix and grade any abnormalities if present.
What happens during the procedure
During a colposcopy, the cervix is visualised using a speculum and is examined under magnification and bright light to look for signs of any abnormality.
Two dyes are applied to the cervix (acetic acid and iodine) which highlight the abnormality if present. From the colposcopy appearance, the abnormalities can also be graded as low grade (CIN1) and high grade changes (CIN2-3).
The colposcopy examination is carried out by a specialist gynaecologist who is accredited by the British Society of Colposcopy and Cervical Pathology (BSCCP).
Sometimes, a colposcopy is performed for assessment after having one of the below symptoms:
- bleeding after sex
- persistent vaginal discharge
- if your GP is concerned about the appearance of your cervix
The examination itself usually takes around 5-7 minutes. You will be able to go home and back to work straight away.
What will the colposcopy show?
The examination may show a normal cervix or low grade or high-grade changes. Your specialist will explain the findings. Depending on your clinical circumstances, you may or may not need treatment.
If I have my period, should I cancel my appointment?
There is no need for cancelling a new colposcopy appointment or treatment appointment as a period will not interfere with the colposcopy assessment. However, if a smear is also required (as in a follow up colposcopy appointment), then it may be better to avoid it during a period.
When would someone need treatment?
It depends on the colposcopy findings and symptoms. All high grade pre-canacerous changes need treatment. Some low grade precancerous changes made need treatment depending on patient choice or if the changes have not regressed within 2 years. Often symptoms particularly vaginal bleeding after sexual intercourse may warrant treatment.
What does the treatment involve?
The commonest form of treatment is LLETZ (Large Loop Excision of Transformation Zone). It is also known as LEEP (Loop Electrosurgical Excision Procedure, an American term). This is commonly carried out as an outpatient clinic procedure under local anaesthesia. After numbing the cervix with local anaesthetic, a wire loop is used to remove the abnormal cells. It is a quick and easy procedure and there is some discomfort, but no sharp pain.
What is CIN?
CIN is an acronym for Cervical Intra-epithelial Neoplasia. These are pre-cancerous changes within the cervical epithelium (lining cells of the neck of womb). There are three grades of CIN (CIN1,2&3) and even CIN3 starts 10 years before cervical cancer. CIN2 & CIN3 are high grade changes and need to be treated to prevent future risk of cervical cancer whereas CIN1 (low grade changes) will often resolve spontaneously.
There are various ways of treating CIN, but the common options are:
LLETZ (Large Loop Excision of Transformation Zone): Also known as LEEP (Loop Electrosurgical Excision Procedure, an American term). This information mainly relates to this procedure.
Cone Biopsy (Extended or deeper excision): Carried out by Laser, Knife or Needle.
When will the results of my colposcopy be available?
Your specialist will discuss the colposcopy findings with you. The results will usually be ready within 10 days.
Is there anything that should be avoided after a colposcopy?
- Nothing if only a colposcopy is performed.
- If a biopsy is also taken, it is best to avoid intercourse, bathing and swimming for 3-4 days. It is ok to shower.
- If you are seen for a colposcopy and treatment, then you should avoid intercourse, swimming, bathing, using tampons or strenuous exercise for a period of 4 weeks.
Can I swim after a colposcopy?
Yes, it is safe to go swimming after a colposcopy unless you have had a biopsy or treatment.
Make an appointment
At London Gynaecology, we offer a range of colposcopy packages which include a 30 minute consultation with a Consultant Gynaecologist as standard and direct access for any urgent health concerns.
If you would like to enquire about a colposcopy or learn more about any of our services please call 0207 10 11 700 or email our team on [email protected]
London Gynaecology is proud to be rated of 4.9/5 overall by patients across Trustpilot, Google and Doctify.



